 Each generation has a nickname –Millenials, Gen X, Baby Boomers, etc. I am a baby boomer and this article is frightening to me. It discusses the tens of thousands of baby boomer Nurses that are starting to retire and will continue to retire over the next few years.
Each generation has a nickname –Millenials, Gen X, Baby Boomers, etc. I am a baby boomer and this article is frightening to me. It discusses the tens of thousands of baby boomer Nurses that are starting to retire and will continue to retire over the next few years.Beginning in the early 1970s, career-oriented and largely female baby boomers embraced the nursing profession in unprecedented numbers following large increases in health care spending after the introduction of the Medicare and Medicaid programs. By 1990, baby-boomer registered nurses (RNs) numbered nearly one million and comprised about two-thirds of the RN workforce. As these RNs aged over the next two decades, they accumulated substantial knowledge and clinical experience. The number of boomer RNs peaked at 1.26 million in 2008, and, after a brief delay in the early part of the current decade (likely associated with the Great Recession), the baby-boomer RN cohort began retiring in large numbers. Since 2012, roughly 60,000 RNs exited the workforce each year, and by the end of the decade more than 70,000 RNs will be retiring annually. In 2020, baby-boomer RNs will number 660,000, roughly half their 2008 peak.
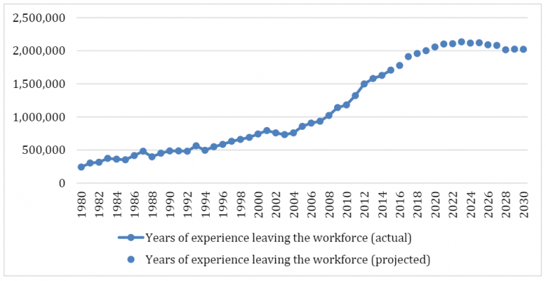
The retirement of one million RNs from the nursing workforce between now and 2030 will mean that their accumulated years of nursing experience leave with them. We estimate that the number of experience-years lost from the nursing workforce in 2015 was 1.7 million (multiplying the number of retiring RNs by the cumulative years of experience for each RN), double the number from 2005 (see Figure 1). This trend will continue to accelerate as the largest groups of baby-boomer RNs reach their mid to late sixties. The departure of such a large cohort of experienced RNs from the workforce means that patient care settings and other organizations that depend on RNs will face a significant loss of nursing knowledge and expertise that will be felt for many years to come.
The exit and replacement of retiring RNs will not occur uniformly because health care delivery organizations in some regions of the country will confront faster RN retirements and slower replacements of their RN workforce (especially the New England and Pacific regions) compared to other regions of the country (the Southern and Central regions). Consequently, some organizations will experience bursts in RN retirements that may result in temporary nursing shortages and disruptions in care delivery. How can health care delivery organizations overcome the loss of so much nursing knowledge, wisdom, and expertise?
Health care leaders must recognize that the retirement of the RN workforce has only recently begun, that it will intensify over the coming years, and that the loss of RNs with decades of experience creates multiple risks. Foremost, the quality of patient care could decrease as new and less experienced RNs enter the workforce and replace RNs with decades of experience. This is not to suggest that RNs with fewer years of nursing experience are less qualified to provide high-quality nursing care. Rather, it is to acknowledge that the longer an RN is in the workforce, the knowledge accumulated over many years is likely to increase a nurse’s ability to effectively manage all types of clinical and organizational challenges.
Relative to novice RNs, experienced RNs are likely to be more adept at identifying complications and unexpected changes in patient conditions sooner and respond appropriately. They are also more likely to know how to manipulate the organization’s culture to “get things done,” make clinical assignments that better match the knowledge and skills of nurses with the needs of the patient, serve as role models and mentors, and deal effectively with physicians, administrators, and others to assure the well-being of patients and their families. All of these attributes can matter greatly in providing a consistent, predictable, and safe patient environment. It is not difficult to recognize these nurses—often they are the clinical and organizational leaders who are counted on to ensure smooth operations of clinical and administrative systems.
Health care organizations must also recognize that the retirement of so many experienced RNs will occur commensurate with the aging of the country’s nearly 80 million baby boomers. Not only will growing numbers of elders increase the demand for RNs, but because three in four people older than age 65 have multiple chronic diseases, the intensity of nursing care required to manage this medically complicated population will also increase. Aging baby boomers will especially benefit from care provided by the most experienced nurses—the very nurses who are retiring from the workforce.
Four actions should be taken by hospital chief nursing executives, hospital patient care unit managers, and human resource officers to both anticipate and act to prevent the negative consequences that could ensue as RN retirement accelerates.
First, it is important to gather information on an organization’s nursing workforce to ascertain when and how many RNs are expected to retire and identify the nursing units, departments, and patient populations that will be affected. Sharing this information with physicians and other clinicians who will be affected and seeking their involvement will be critical to mitigating potential harmful consequences.
Second, hospital leadership should prioritize working with department and unit leaders to engage soon-to-be retiring RNs to learn what can be done to delay their retirement—for example, decreasing hours and number of workdays, modifying their responsibilities, improving the ergonomic environment to minimize injuries, or revising organizational policies and clinical conditions that hinder and dissatisfy nurses. Similarly, older and more experienced RNs could be offered opportunities to fill new roles in community engagement, patient navigation, or education and prevention.
Third, it is important to encourage the creation of programs that bring older and younger RNs together to identify the knowledge and skills needed by rising RNs that can be imparted by older and more experienced RNs. Fourth, review (and strengthen as needed) succession planning to assure that retiring nursing managers will be replaced by RNs who are well-prepared to assume management of clinical and administrative operations on patient care units. Future RN leaders could be identified and partnered with soon-to-be retiring RNs in management positions and participate in formal programs in management and leadership development, team building, communications, budgeting, program development, and other leadership roles.
It is imperative that health care leaders recognize that as the retirement of RNs ramps up, a different type of nursing shortage will emerge—one of knowledge, skill, experience, and judgment, all attributes that contribute to the successful clinical and administrative operations of complex health care delivery systems. Now is the time to anticipate and prepare for the retirement wave of the nation’s RN workforce.
Figure 1. Number Of Years Of Experience Lost To The Registered Nurse Workforce, 1979-2030



 As Baby Boomers age into retirement by the millions each year, their growing health care needs require more people to administer that care.
As Baby Boomers age into retirement by the millions each year, their growing health care needs require more people to administer that care.
